You just finished a bowl of pasta. Within 30 minutes, your blood glucose will spike to its peak, potentially reaching 160 to 180 mg/dL even if you have no history of diabetes. That spike triggers an insulin surge, which overshoots and drives your blood sugar below baseline an hour later, leaving you foggy, irritable, and reaching for a snack. This postprandial rollercoaster happens two to three times every day, and over years, those repeated glucose spikes contribute to insulin resistance, arterial damage, and chronic inflammation, the metabolic groundwork for type 2 diabetes and cardiovascular disease.
Now imagine you put on your shoes and walk around the block after that pasta. A 2025 randomized controlled trial from Ritsumeikan University in Japan, published in Scientific Reports, found that just 10 minutes of walking immediately after a glucose load reduced peak blood sugar levels significantly compared to remaining seated. The 10-minute walk produced glucose areas under the curve of 15,607 mg-min/dL versus 16,605 mg-min/dL in the sedentary control, a meaningful reduction achieved with the simplest possible intervention: putting one foot in front of the other.
Postprandial walking is not a new idea. But the research supporting it has matured substantially over the past three years, and the emerging consensus on timing, duration, and intensity is more specific and more actionable than ever before.
Why Post-Meal Glucose Spikes Matter (Even If You’re Healthy)
If you don’t have diabetes, you might assume that blood sugar management isn’t your problem. That assumption is increasingly outdated. Continuous glucose monitor (CGM) data from non-diabetic populations has revealed that “healthy” people experience glucose spikes above 140 mg/dL regularly, and that the frequency and magnitude of those spikes correlate with long-term metabolic risk independent of fasting glucose or HbA1c levels.
The damage from glucose spikes operates through several mechanisms. When blood sugar rises rapidly, it overwhelms the endothelium (the inner lining of blood vessels), generating reactive oxygen species that damage arterial walls. Repeated spikes promote glycation, a process where glucose molecules bind to proteins and lipids, forming advanced glycation end products (AGEs) that accelerate aging of blood vessels, kidneys, and nerves. The insulin surges triggered by each spike, meanwhile, promote fat storage and contribute to progressive insulin resistance when they occur chronically.
Research from Dr. Loretta DiPietro at George Washington University, published in Diabetes Care, demonstrated that even in older adults at risk for impaired glucose tolerance (but not yet diabetic), three 15-minute post-meal walks per day significantly improved 24-hour glycemic control compared to a single sustained 45-minute walk. The post-meal timing was critical: the same total exercise volume produced better glucose management when distributed around meals rather than performed in a single session unrelated to eating.
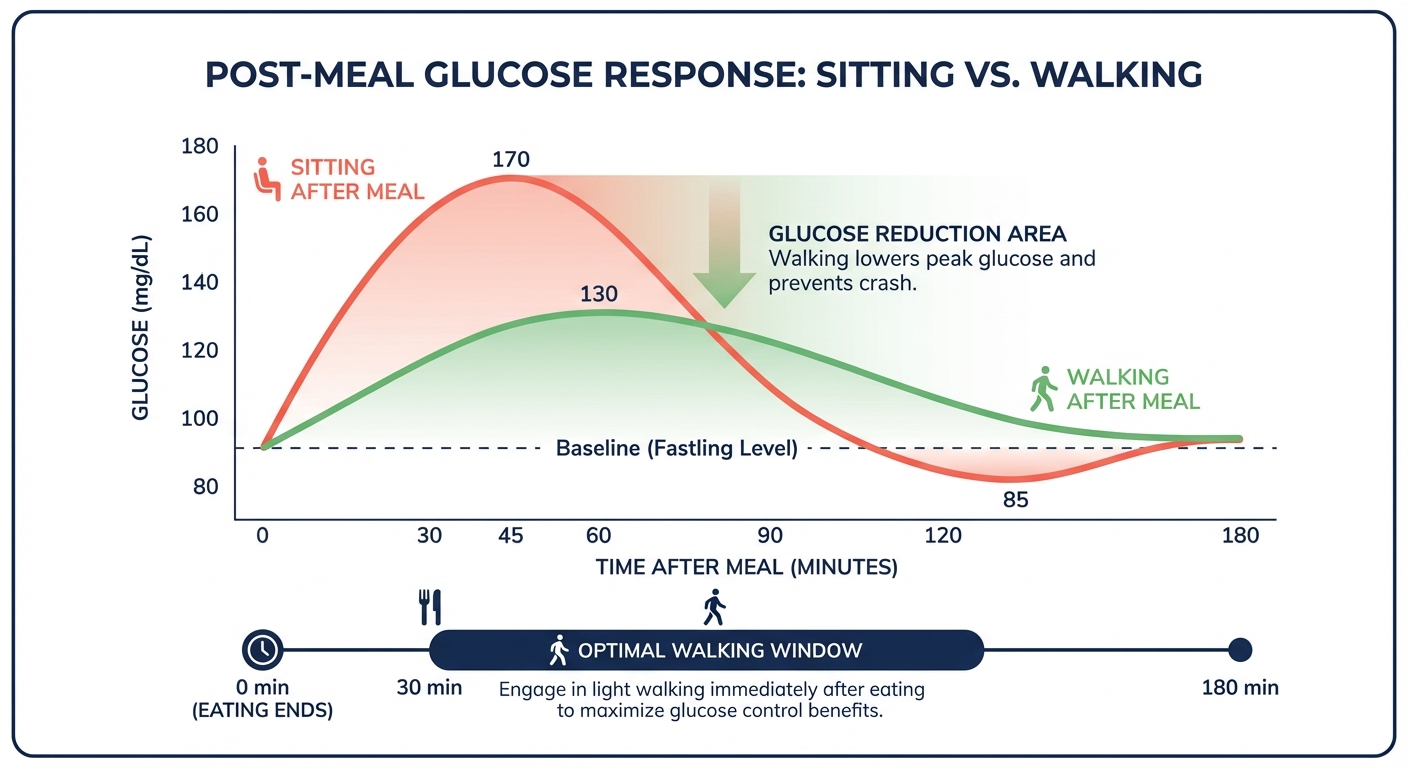
The takeaway is that glucose management isn’t just for diabetics. It’s a fundamental aspect of metabolic health that affects energy levels, cognitive function, body composition, and long-term disease risk. And the simplest intervention, the one with the lowest barrier to entry and essentially zero risk, is walking after you eat.
The Optimal Timing Window: Sooner Is Better
One of the most clinically relevant findings in the postprandial exercise literature is that timing matters more than most people realize. The same walk produces different results depending on when you take it relative to your meal.
A 2018 randomized controlled trial published in Nutrients, testing activity timing in healthy adults, found that light walking commenced immediately after a meal or within 30 minutes of the start of eating significantly lowered postprandial blood glucose. But delaying the start of activity by one hour eliminated the glycemic benefit entirely. The walkers who waited 60 minutes showed glucose responses indistinguishable from the sedentary control group.
A 2023 systematic review with meta-analysis, published in Sports Medicine, confirmed this pattern across multiple studies. Exercise performed in the early postprandial phase (0 to 29 minutes after eating) produced the largest reductions in glucose excursions. Exercise initiated 30 to 120 minutes after eating showed a trend toward smaller effects. The physiological explanation is straightforward: glucose absorption from the small intestine peaks approximately 30 to 60 minutes after eating. Walking during this window activates skeletal muscle glucose uptake through a pathway (GLUT4 transporter translocation) that is independent of insulin. Your muscles pull glucose directly from the bloodstream to fuel the walking, effectively competing with the glucose influx from digestion and flattening the spike.
The practical guideline: start your walk within 15 to 30 minutes of finishing your meal. Immediately after eating is ideal, but you don’t need to sprint out the door. Finishing your meal, clearing the table, putting on shoes, and heading out the door is about the right pace. The key is not to sit down on the couch first, because if you do, you’ll likely still be sitting there when the optimal window closes.
How Long and How Fast: The Dose-Response Evidence
The research on duration presents a surprisingly encouraging picture for people who feel they don’t have time for exercise.
A meta-analysis of seven studies, covered by CNN and UCLA Health, found that as little as two to five minutes of walking after a meal produced measurable reductions in blood sugar compared to remaining seated. The benefits increased with duration up to about 15 to 30 minutes, after which additional time provided diminishing returns for glucose control specifically.
The 2025 Ritsumeikan University study offers a particularly interesting comparison. Researchers tested two walking conditions against a sedentary control: a 10-minute walk starting immediately after glucose ingestion, and a 30-minute walk starting 30 minutes after ingestion. Both walking conditions produced significantly lower mean blood glucose levels (127.9 mg/dL and 128.9 mg/dL respectively) compared to the control (135.8 mg/dL). But the 10-minute immediate walk was the only condition that significantly reduced peak glucose levels. The 30-minute delayed walk improved average glucose but didn’t blunt the spike as effectively, because the peak had already occurred before the walk began.

Intensity, perhaps surprisingly, matters less than timing. The participants in the Ritsumeikan study walked at a self-selected comfortable pace averaging 3.8 km/h (about 2.4 mph), which is a casual stroll, not a power walk. A study published in the Journal of the International Society of Sports Nutrition found that modulating exercise intensity from light to moderate did not produce substantial variation in postprandial glucose responses in healthy individuals. The primary driver of the glucose-lowering effect is the activation of skeletal muscle, which occurs at any walking speed. You don’t need to break a sweat. You just need to move.
The practical prescription:
- Minimum effective dose: 2 to 5 minutes of walking, starting immediately after eating
- Sweet spot: 10 to 15 minutes of comfortable walking, starting within 15 minutes of finishing your meal
- Optimal if you have time: 15 to 30 minutes at a moderate pace
Walking Versus Other Post-Meal Activities
If walking works by activating skeletal muscle, does standing accomplish the same thing? What about other forms of light activity?
A systematic review and meta-analysis comparing sitting, standing, and walking after meals found that standing did reduce glucose levels compared to prolonged sitting, but the effect was far more modest. Intermittent standing breaks throughout the day reduced glucose by an average of 9.51% compared to prolonged sitting, while intermittent light-intensity walking reduced glucose by 17.01%. Walking was roughly twice as effective as standing for glucose management.
The difference makes physiological sense. Standing activates postural muscles at low intensities, which does create some glucose demand, but walking engages the large muscle groups of the legs (quadriceps, hamstrings, glutes, and calves) through a full range of motion, creating substantially greater glucose uptake per minute. The rhythmic contraction-relaxation cycle of walking also enhances blood flow to working muscles, which improves glucose delivery and clearance simultaneously.
Other forms of light post-meal activity, such as gentle stretching, slow cycling, or light housework, likely provide benefits similar to walking, though the evidence base is thinnest for these alternatives. The advantage of walking is its accessibility: it requires no equipment, no special clothing, no gym membership, and no instruction. You can do it in dress shoes, in an office building, on a sidewalk, or in a shopping mall. It is the lowest-friction exercise intervention in existence.
Building the Post-Meal Walking Habit: A Practical Protocol
The research is clear. The challenge is behavioral: turning a single walk after dinner into a consistent daily habit. Here’s a structured approach based on behavior change science and the dose-response data.
Week 1 to 2 (Foundation): Walk for 5 to 10 minutes after your largest meal of the day. For most people, this is dinner. Don’t add walks after other meals yet. The goal is to establish one consistent trigger-action pair: finish dinner, then walk. Keep your walking shoes by the door. Set a phone reminder for 5 minutes after your typical dinner time.
Week 3 to 4 (Expansion): Add a second post-meal walk, either after lunch or breakfast, depending on your schedule. Keep the duration at 5 to 10 minutes. The barrier should feel almost negligibly low.
Week 5 onward (Optimization): Aim for three post-meal walks per day (after each main meal) of 10 to 15 minutes each. This matches the protocol in Dr. DiPietro’s Diabetes Care study, which showed significant 24-hour glycemic improvement in at-risk older adults. If three walks per day isn’t realistic, prioritize the walk after your highest-carbohydrate meal, which is where the largest glucose spike occurs.
Troubleshooting common obstacles:
If the weather is bad, walk indoors. A few laps around your house, up and down a hallway, or on a treadmill provides the same metabolic benefit. The stimulus is skeletal muscle activation, not fresh air.
If you eat at your desk, take a “walking meeting” or phone call immediately after eating. The social or work context makes the walking feel purposeful rather than like an additional chore.
If you have digestive discomfort from walking immediately after eating, wait 5 to 10 minutes, then start at a gentle pace. Most people find that light walking actually aids digestion by stimulating gastric motility, but if you experience cramping, a slower pace resolves it without sacrificing the glucose benefit.
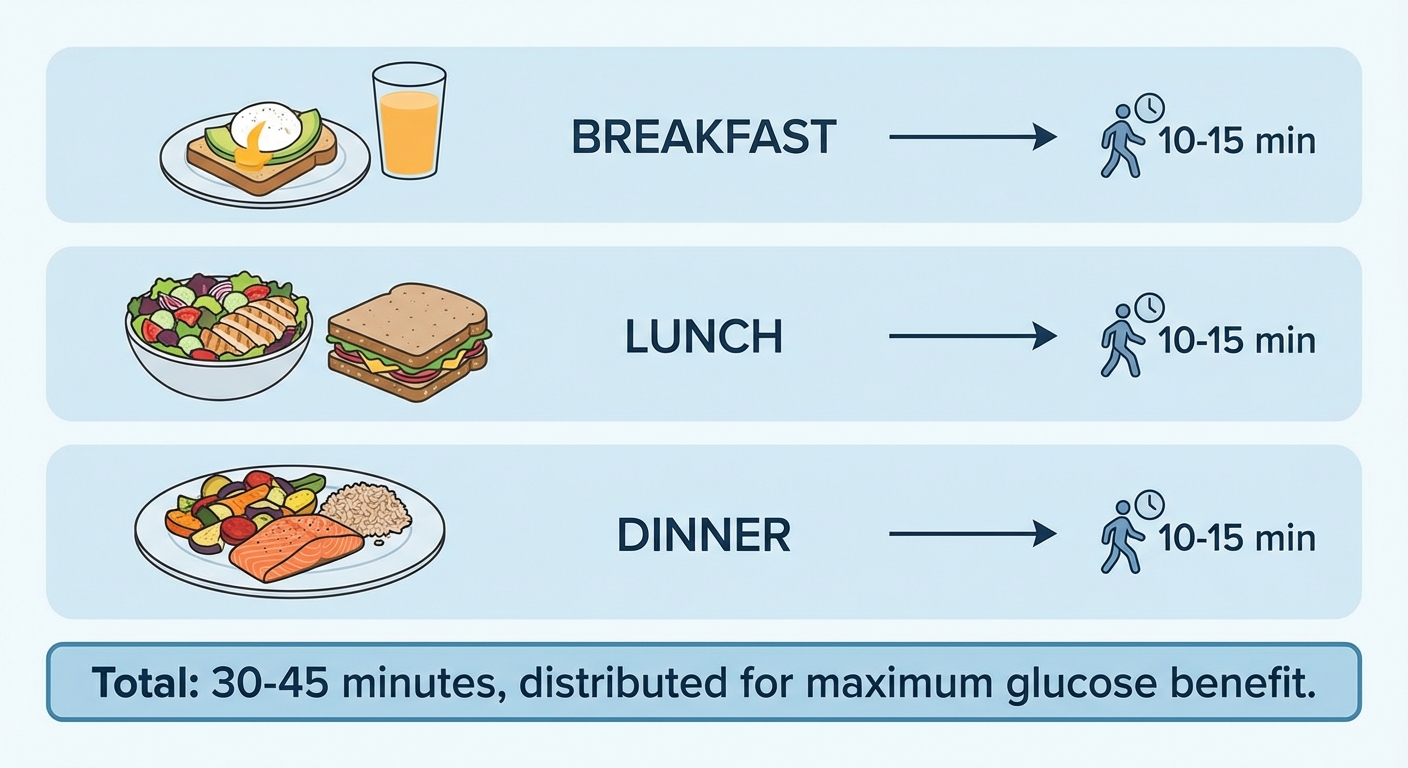
The Compounding Returns of a Simple Walk
The glucose-lowering effect of postprandial walking is immediate and measurable after a single meal. But the long-term metabolic benefits compound in ways that extend well beyond blood sugar management. Regular post-meal walking improves insulin sensitivity over weeks, meaning your body requires less insulin to handle the same glucose load. It supports healthy body composition by redirecting dietary glucose toward working muscles rather than fat storage. It reduces the chronic low-grade inflammation associated with metabolic syndrome and cardiovascular disease. And it accumulates significant daily step counts (three 10-minute walks add roughly 3,000 to 4,000 steps) without requiring a dedicated “workout” that many people struggle to fit into their schedules.
What makes this intervention remarkable isn’t its potency. It’s the ratio of benefit to effort. You’re not being asked to train for a marathon, buy a gym membership, or learn complex exercise programming. You’re being asked to walk for 10 minutes after you eat. The research shows that this simple, ancient human behavior, something our ancestors did as a matter of course, produces metabolic benefits that pharmaceutical interventions struggle to match for side-effect profile and adherence.
Start tonight. Finish dinner. Walk around the block. Your blood sugar will be lower than it would have been. Do it again tomorrow, and the day after that. In a few weeks, you won’t think of it as a health intervention. You’ll think of it as what you do after dinner. That’s the point. The best metabolic health strategy is the one that disappears into your daily routine.
Sources
- Ritsumeikan University. “Positive Impact of a 10-Min Walk Immediately After Glucose Intake on Postprandial Glucose Levels.” Scientific Reports, 2025.
- DiPietro, L. et al. “Three 15-Min Bouts of Moderate Postmeal Walking Significantly Improves 24-h Glycemic Control in Older People at Risk for Impaired Glucose Tolerance.” Diabetes Care, 2013.
- Francois, M.E. et al. “The Timing of Activity After Eating Affects the Glycaemic Response of Healthy Adults: A Randomised Controlled Trial.” Nutrients, 2018.
- Bellini, A. et al. “The Effects of Postprandial Walking on the Glucose Response After Meals with Different Characteristics.” Nutrients, 2022.
- UCLA Health. “Taking a Walk After Eating Can Help with Blood Sugar Control.” 2022.






