She was 72 when her husband of 48 years died of a sudden cardiac arrest at the breakfast table. Three weeks later, she was in the emergency room herself, clutching her chest, convinced she was having a heart attack. The ECG showed something stranger: her left ventricle had ballooned into a shape resembling a Japanese octopus trap, a takotsubo pot. Her coronary arteries were clean. Her heart muscle wasn’t dying from blocked blood flow. It was stunned, temporarily paralyzed by a flood of stress hormones triggered by grief. The cardiologist told her she had “broken heart syndrome.” He wasn’t being poetic. He was giving her a clinical diagnosis.
Takotsubo cardiomyopathy is one of the most dramatic demonstrations of something that cardiovascular researchers have spent decades documenting: your relationships don’t just affect how you feel. They physically reshape your heart, your blood vessels, and your odds of surviving to old age. The evidence has grown strong enough that in 2022, the American Heart Association issued a formal scientific statement declaring social isolation and loneliness associated with approximately a 30% increased risk of heart attack or stroke, placing them alongside smoking, obesity, and physical inactivity as threats to cardiac health.
This Valentine’s Day, the science of love and the science of cardiology have more overlap than a greeting card company could imagine.
Your Heart on Love: The Oxytocin Connection
When you hold your partner’s hand, hug a close friend, or play with your child, your hypothalamus releases oxytocin, a peptide hormone that has been reductively nicknamed the “love hormone” but functions more accurately as a social bonding and physiological regulation signal. What makes oxytocin particularly interesting to cardiologists is that it doesn’t just make you feel warm and connected. It acts directly on the cardiovascular system in ways that are measurably protective.
Research published in Biological Psychology found that higher baseline oxytocin levels correlate with greater vasodilation (blood vessel relaxation), increased cardiac stroke volume, and lower plasma norepinephrine levels during stress. In practical terms, people with more oxytocin circulating in their blood had hearts that pumped more efficiently and blood vessels that stayed more relaxed when confronted with stressful tasks. Their sympathetic nervous system, the fight-or-flight branch, was less reactive. The cardiovascular system behaved as though it had a built-in buffer against stress.
A 2022 study from Michigan State University, published in Frontiers in Cell and Developmental Biology, pushed the oxytocin story even further. Researchers led by Aitor Aguirre discovered that oxytocin stimulates cells in the epicardium (the outer layer of the heart) to migrate inward and differentiate into cardiomyocyte-like progenitor cells, essentially transforming mature cardiac cells into stem-like cells capable of replacing heart tissue damaged by a heart attack. In zebrafish models, oxytocin signaling was essential for cardiac regeneration. The finding suggests that the same hormone released during close social bonding may play a role in the heart’s ability to repair itself after injury.
This doesn’t mean that cuddling can cure a heart attack. The research is preclinical, conducted in animal models and cell cultures. But the biological plausibility is striking: the hormone most strongly associated with human bonding appears to have direct cardioprotective and potentially cardioregenerative properties. The question isn’t whether oxytocin affects the heart. It’s how much of the cardiovascular benefit observed in people with strong social bonds is mediated through this specific pathway versus other mechanisms.
When Loneliness Becomes a Cardiac Risk Factor
If love protects the heart, isolation damages it, and the magnitude of the damage is larger than most people realize. A 2024 systematic review and meta-analysis published in Scientific Reports, analyzing data from over 100,000 patients across multiple studies, found that poor social relationships were associated with a 16% increase in the risk of incident cardiovascular disease. Among older adults specifically, individuals with poor social health were 42% more likely to develop CVD and twice as likely to die from cardiovascular causes over a median 4.5-year follow-up.
The American Heart Association’s 2022 scientific advisory, authored by a panel of experts and published in the Journal of the American Heart Association, reviewed the accumulated evidence and concluded that social isolation and loneliness should be formally assessed as risk factors during cardiovascular health evaluations. The advisory noted that approximately one in four adults over 65 reports social isolation, and the prevalence of loneliness in the United States has been rising steadily for decades.
What makes social isolation dangerous at the biological level is the chronic activation of the body’s stress response systems. When humans perceive themselves as socially disconnected, the hypothalamic-pituitary-adrenal (HPA) axis remains in a heightened state, producing sustained elevation of cortisol and inflammatory markers. Research by Dr. Steve Cole at UCLA has identified a specific pattern of gene expression in lonely individuals, called the “conserved transcriptional response to adversity” (CTRA), that upregulates inflammatory genes and downregulates antiviral immune genes. This chronic inflammatory state accelerates atherosclerosis, the buildup of plaque in arterial walls that underlies most heart attacks and strokes.
The cardiovascular system evolved to treat social isolation as a danger signal. In ancestral environments, being separated from your group meant vulnerability to predation and reduced access to resources. The stress response to isolation was adaptive when it was temporary, pushing the isolated individual to seek reconnection. But in modern life, where loneliness can persist for months or years, that same stress response becomes a slow-acting poison for the cardiovascular system.
Broken Heart Syndrome: When Grief Attacks the Heart
Takotsubo cardiomyopathy, the condition that brought our 72-year-old widow to the emergency room, provides the most vivid evidence that emotional states can directly damage cardiac function. First described in Japan in 1990, the condition occurs when an intense emotional or physical stressor triggers a surge of catecholamines (adrenaline and noradrenaline) that temporarily stun the heart muscle, causing the left ventricle to balloon outward and lose its ability to pump effectively.
A 2024 study published in the Journal of the American Heart Association, analyzing national data from 2016 to 2020, found that Takotsubo remains a significant cause of cardiac morbidity with persistently high complication rates including heart failure, atrial fibrillation, and stroke. The study revealed a striking gender disparity: men with Takotsubo had more than double the mortality rate compared to women, despite women accounting for approximately 90% of cases. The emotional triggers most commonly associated with the condition include the death of a loved one, relationship dissolution, and severe interpersonal conflict.
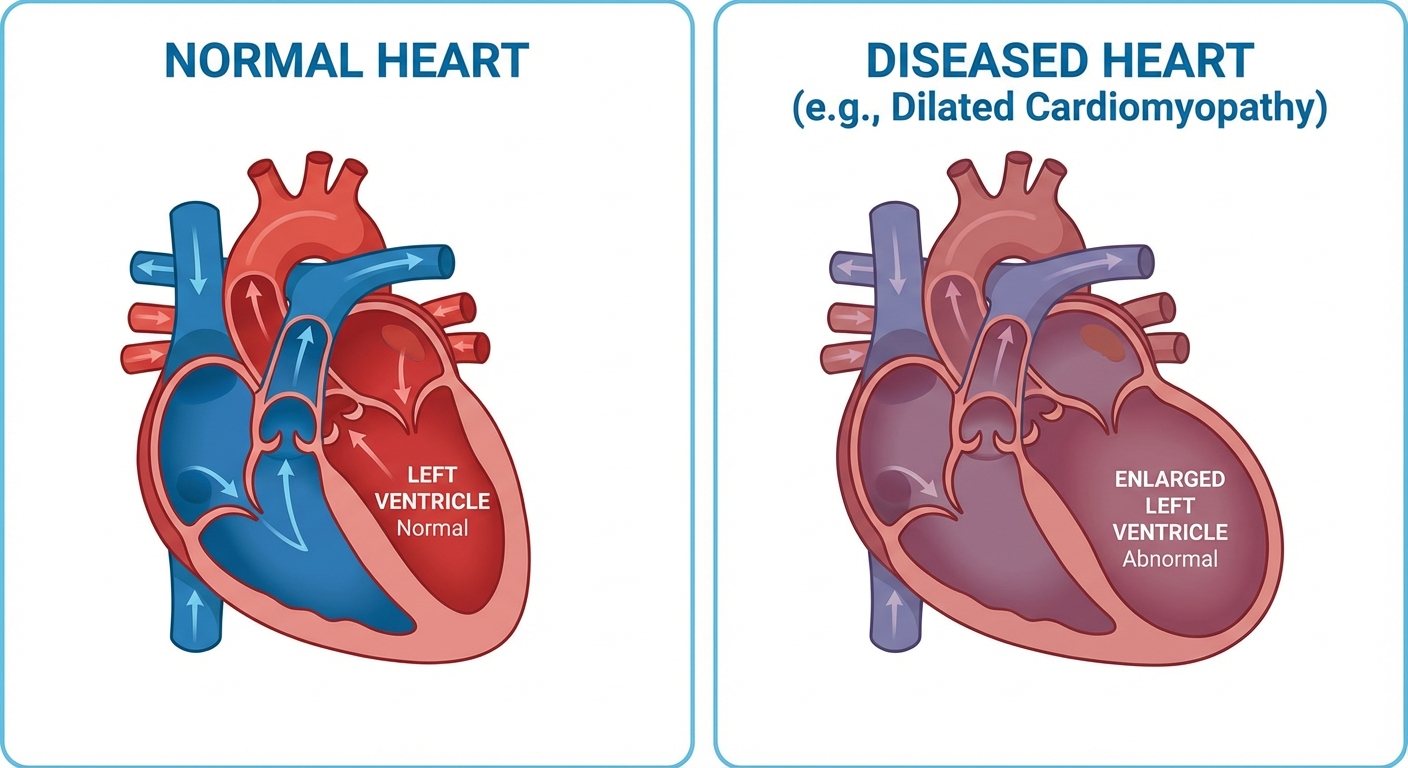
A scoping review published in PMC examined the specific connection between loneliness, social isolation, and Takotsubo syndrome. The researchers found that both loneliness and social isolation are associated with exaggerated autonomic stress responses and sympathetic nervous system hyperactivity, which lead to increased total peripheral resistance, reduced heart rate variability, hypertension, and diminished cardiac output. These are precisely the physiological conditions that prime the heart for a Takotsubo event. The implication is that chronic loneliness doesn’t just increase the risk of gradual cardiovascular disease; it may make the heart more vulnerable to acute stress-induced cardiac events.
The Marriage Effect: Partnership and Cardiac Survival
Population-level data on marriage and cardiovascular outcomes has been remarkably consistent across cultures and decades. Multiple large studies have found that married individuals have lower rates of cardiovascular disease, better survival after cardiac events, and reduced all-cause mortality compared to their unmarried counterparts.
The mechanism appears to operate through several pathways simultaneously. Partners provide practical support that affects health behaviors: reminding each other to take medications, encouraging physical activity, preparing healthier meals, and noticing symptoms that the affected person might ignore. But the benefits extend beyond logistics. The physiological co-regulation that occurs between bonded partners, where close physical proximity and emotional attunement influence each other’s nervous system activity, heart rate variability, and cortisol rhythms, creates a biological environment that is directly cardioprotective.
Research on vagal tone, the activity level of the vagus nerve that governs parasympathetic function, shows that people in satisfying relationships tend to have higher resting vagal tone. Higher vagal tone is associated with lower resting heart rate, greater heart rate variability (a marker of cardiovascular resilience), reduced inflammation, and better blood pressure regulation. When partners are in physical proximity, their physiological rhythms tend to synchronize, a phenomenon researchers call “co-regulation.” Studies using simultaneous heart rate and respiratory monitoring have found that partners’ cardiac rhythms begin to align during close interaction, with the more physiologically calm partner effectively bringing the more stressed partner’s system toward equilibrium.
The critical caveat is that relationship quality matters enormously. A conflictual, hostile, or emotionally abusive relationship does not confer cardiovascular protection. Research consistently shows that marital distress is associated with increased cardiovascular reactivity, higher inflammatory markers, and poorer cardiac outcomes. The protective effect comes from the quality of connection, not the legal status of the relationship itself. Close friendships, strong family bonds, and community ties provide similar (though sometimes smaller) cardiovascular benefits, confirming that the underlying mechanism is social connection rather than marriage per se.
Beyond Romance: Building a Heart-Healthy Social Life
The cardiovascular benefits of social connection aren’t exclusive to romantic partnerships, which matters enormously for the roughly 50% of American adults who are single at any given time. A meta-analysis published in BMC Geriatrics analyzing data from multiple prospective cohort studies found that social support and community engagement independently predicted lower cardiovascular disease incidence and mortality, regardless of marital status.
The key factor appears to be the depth and regularity of social interaction rather than its type. Meaningful conversation, shared activities, physical touch (handshakes, hugs, pats on the back), and reliable emotional support all trigger oxytocin release and parasympathetic activation. Regular physical activity performed in social settings, such as walking groups, group fitness classes, or recreational sports leagues, may offer compounded cardiovascular benefits by combining the protective effects of exercise with the protective effects of social connection.

Volunteer work, religious or spiritual community participation, and even regular interactions with neighbors have all shown associations with improved cardiovascular markers in observational studies. The dose appears to matter: some research suggests that three or more meaningful social interactions per week represents a threshold below which cardiovascular risk begins to increase. This doesn’t mean brief pleasantries in the elevator count. It means sustained, engaged interaction where genuine emotional exchange occurs.
For individuals who are currently socially isolated, the research suggests a graduated approach. Dr. Julianne Holt-Lunstad, a professor of psychology and neuroscience at Brigham Young University whose meta-analyses have been foundational in establishing the mortality impact of social isolation, recommends treating social connection as a health behavior, something you prioritize and schedule the same way you would exercise or sleep. Start with one additional social interaction per week, whether that’s joining a class, calling a friend, or volunteering. The physiological benefits of social connection begin accruing immediately, just as the physiological benefits of exercise begin with the first session.
The Co-Regulation Advantage: An Original Framework
What the research on love and cardiovascular health reveals, when synthesized across disciplines, is something that individual studies rarely state explicitly: the heart is not a solo organ. It evolved within a social species, and its regulatory systems are designed to function optimally in the context of close social bonds. This is what I call the “co-regulation advantage,” and it reframes how we think about cardiovascular health.
Traditional cardiology focuses on individual risk factors: your cholesterol, your blood pressure, your weight, your diet. These matter enormously. But the co-regulation framework suggests that your cardiovascular system has a built-in dependency on external social input. Your vagal tone is partly regulated by the presence and behavior of people you’re bonded to. Your cortisol rhythm is influenced by the emotional climate of your close relationships. Your inflammatory gene expression shifts based on whether you perceive yourself as socially connected or isolated. The heart, in a meaningful biological sense, is a relational organ.
This framework explains several otherwise puzzling findings in cardiology. It explains why widowhood carries a measurably elevated cardiac risk in the months following a spouse’s death, sometimes called the “widowhood effect,” that exceeds what grief-related behavioral changes (poor diet, missed medications, reduced activity) can account for. It explains why cardiac rehabilitation programs that include group support components produce better outcomes than identical programs delivered individually. And it explains why social isolation produces cardiovascular damage through inflammatory pathways that mirror chronic infection, as if the body is responding to a perceived biological threat rather than merely a psychological discomfort.
The practical implication is that cardiovascular health is partly a social project. You can eat perfectly, exercise optimally, manage your weight, and control your cholesterol, but if you are chronically socially isolated, you are leaving a significant and modifiable risk factor unaddressed.
Your Heart Health Action Plan
The evidence connecting social bonds to cardiovascular outcomes is strong enough to warrant specific, measurable action, not just a vague resolution to “be more social.”
Prioritize relationship quality over quantity. One or two deeply supportive relationships provide more cardiovascular benefit than a large but superficial social network. Invest in the connections where genuine emotional exchange occurs. If a relationship is consistently conflictual or hostile, recognize that it may be actively harmful to your cardiovascular health, not just your mood.
Schedule social connection like exercise. Aim for at least three meaningful social interactions per week. This can include phone calls, shared meals, walking with a friend, group activities, or volunteering. The key is regularity and emotional depth, not duration.
Use physical touch intentionally. Hugging, hand-holding, and other forms of affectionate touch trigger oxytocin release and parasympathetic activation. If you’re in a partnership, brief physical contact throughout the day (a six-second hug, holding hands during a walk) accumulates cardiovascular benefit over time.
Combine social connection with physical activity. Walking groups, recreational sports, and group fitness classes deliver dual cardiovascular benefits. Even replacing one solo workout per week with a social one adds the protective effects of connection to the protective effects of exercise.
Address isolation proactively. If you recognize yourself as socially isolated, treat it with the same seriousness you would treat high blood pressure. Join one group, class, or volunteer organization. Call one person per week. The physiological response to reconnection begins quickly, and compounds over time.
Your heart doesn’t beat in isolation. It beats in the context of your relationships, your community, and the quality of connection that surrounds you. The science of love, it turns out, is also the science of survival.
Sources
- American Heart Association. “Effects of Objective and Perceived Social Isolation on Cardiovascular and Brain Health.” Scientific Statement, Journal of the American Heart Association, 2022.
- Nature. “The Impact of Social Isolation and Loneliness on Cardiovascular Disease Risk Factors: A Systematic Review, Meta-analysis, and Bibliometric Investigation.” Scientific Reports, 2024.
- Wasserman, A.H. et al. “Oxytocin Promotes Epicardial Cell Activation and Heart Regeneration After Cardiac Injury.” Frontiers in Cell and Developmental Biology, 2022.
- PMC. “The Role of Oxytocin in Cardiovascular Protection.” International Journal of Molecular Sciences, 2020.
- BMC Geriatrics. “Social Isolation, Social Support and Loneliness as Predictors of Cardiovascular Disease Incidence and Mortality.” 2021.